Atopic Dermatitis May Start in the Gut, Not the Skin
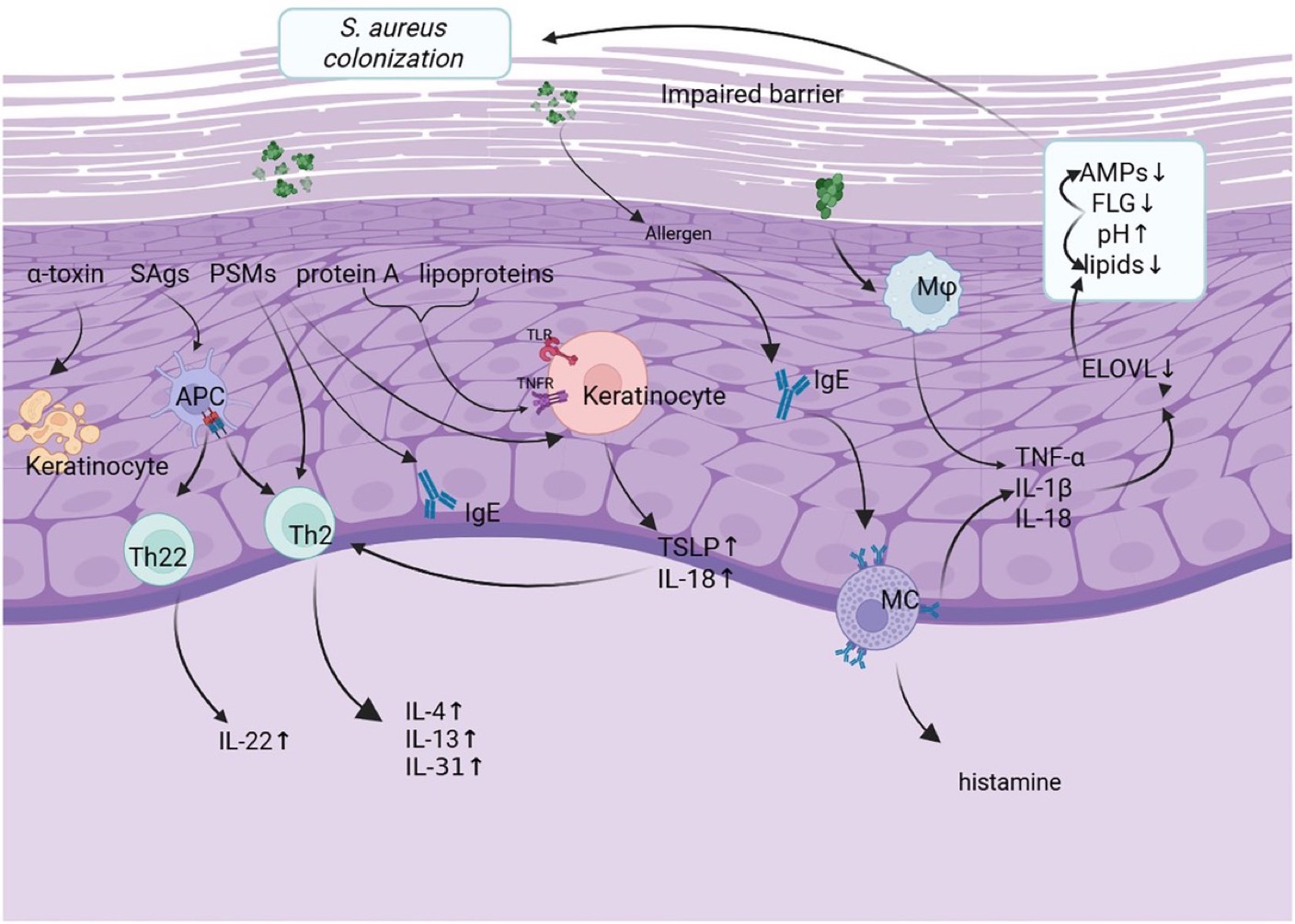
Atopic dermatitis (AD) is a chronic inflammatory skin condition affecting up to 20% of children and 10% of adults worldwide. It has long been treated as a problem of skin barrier defects and immune overreaction. But recent research is shifting the focus from skin to gut.
The Gut-Skin Axis, a Two-Way Connection
The gut-skin axis describes the bidirectional communication pathway between the gut microbiome and skin health. A 2025 review in Gut Microbes analyzed the therapeutic potential of microbe-mediated treatments through this axis.
Microbial imbalance (dysbiosis) in both the skin and gut can contribute to the onset and severity of atopic dermatitis. Overgrowth of pathogenic organisms and suppression of healthy commensal bacteria are the core mechanisms.
Early-Persistent AD and Gut Acetate
A 2025 study produced a notable finding: early-onset, persistent atopic dermatitis was associated with gut acetate levels and Ruminococcus gnavus abundance. This challenges the traditional skin-centric treatment paradigm and highlights the importance of gut-targeted interventions.
Probiotics and Postbiotics
Clinical applications are already underway. The strategy involves restoring gut microbial balance using probiotics, such as Lactobacillus rhamnosus, that modulate Th2 immune responses (the immune pathway linked to atopic conditions). For patients with early-persistent AD, supplementing acetate-producing bacteria (including Ruminococcus gnavus) is a priority consideration.
Postbiotics (microbial metabolites and cell components) are also gaining traction, offering a higher safety profile than live bacterial administration. Fecal microbiota transplantation (FMT) and short-chain fatty acid (SCFA) supplementation are being explored as additional microbiome-targeted therapies.
Early Stage, but the Direction Is Clear
A 2026 review in Frontiers comprehensively analyzed the potential for treating atopic dermatitis through gut microbiome restoration. Current meta-analyses, however, show heterogeneity and possible publication bias, and most trials are small with short follow-up periods.
From a practical standpoint, healthcare professionals are increasingly looking at combining multi-omics data from gut and skin to design personalized treatment plans. Using probiotics and lipid supplements together is one example. This integrative approach is especially emphasized in pediatric patients.
The recognition that atopic dermatitis may not be “just a skin problem” is gaining momentum. Gut health management is increasingly positioned as a core pillar of AD care.