Postbiotics Emerge as a New Paradigm in Acne Management
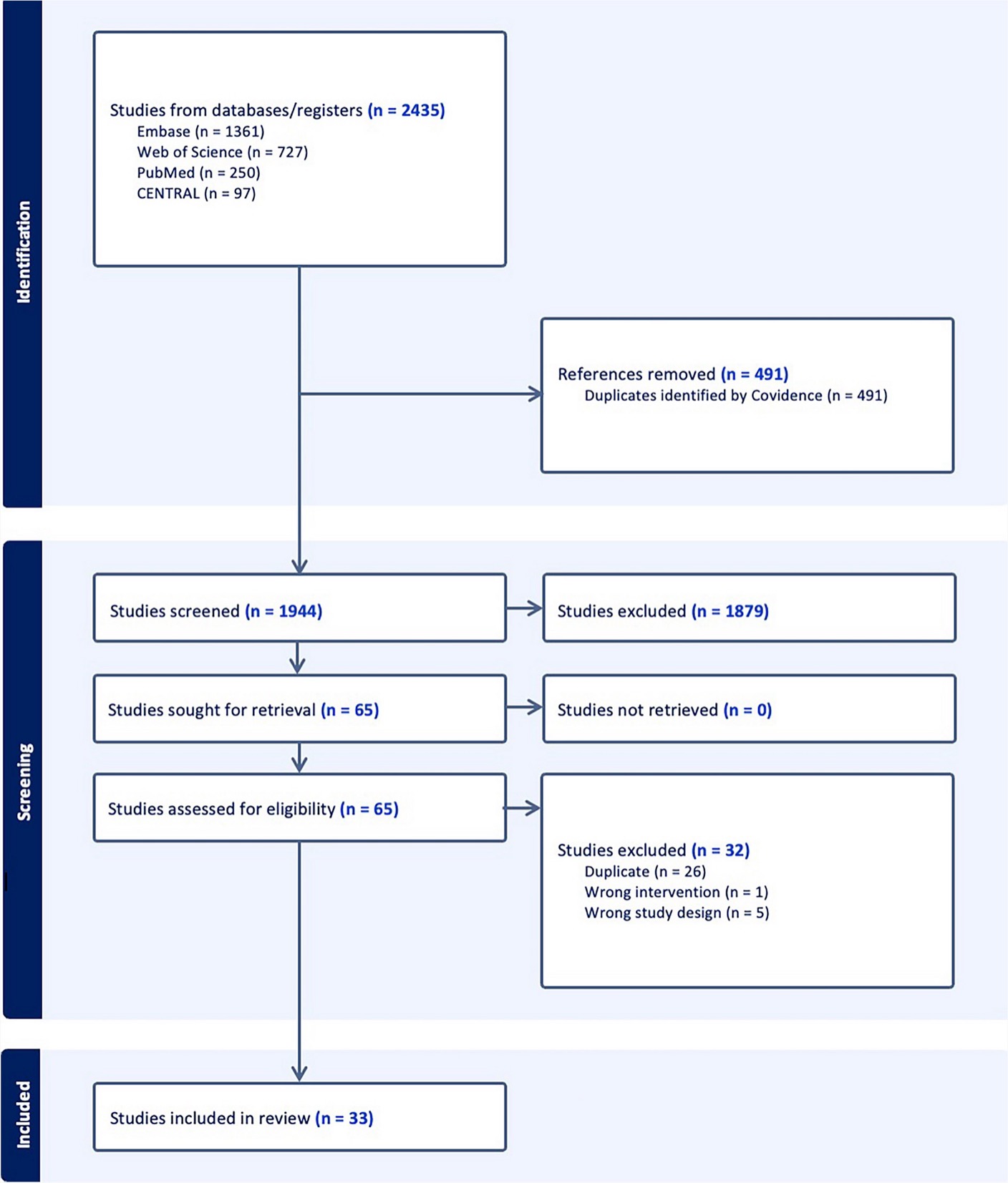
Acne treatment has long centered on antibiotics and retinoids. But growing concerns about antibiotic resistance and microbiome disruption have pushed researchers to explore the gut-skin axis as an alternative route. A 2026 systematic review published in Dermatology and Therapy examined whether prebiotics, probiotics, and postbiotics can serve as supportive tools in acne management.
Gut Microbiota Regulate Skin Inflammation
Acne vulgaris is an inflammatory condition driven by excess sebum production and bacterial proliferation (primarily C.acnes) within hair follicles. Over the past decade, evidence has accumulated showing that gut dysbiosis raises systemic inflammation levels, which in turn worsens skin inflammation. When the gut barrier weakens, endotoxins (LPS) leak into the bloodstream and trigger inflammatory cascades in the skin.
Strain-Specific Skin Effects
The review catalogued strain-level data. Lactobacillus plantarum HY7714, taken orally, improved skin elasticity and reduced wrinkle depth in clinical settings. The proposed pathway involves stimulating ceramide synthesis, which reinforces the skin barrier. L.paracasei CNCM I-5220 showed capacity to suppress skin inflammatory responses and protect barrier function.
In the postbiotic space, early data on Akkermansia muciniphila-derived components suggested potential for skin repair. Akkermansia is known for strengthening the intestinal mucus layer, and the hypothesis is that its metabolites may also support skin barrier recovery.
Hurdles That Remain
The review’s conclusions are cautious. Most studies are small-scale, effects vary by strain, and response differences across acne severity grades have not been mapped. Generalizing that “probiotics help acne” oversteps the current evidence. The field needs precision research defining which strain, at what dose, for which acne subtype.
A Practical Approach
The evidence supports adding gut-skin axis management as a complementary layer, not replacing existing acne treatments. Fermented foods (yogurt, kimchi, kefir) provide a baseline for gut health maintenance. When adding a strain-specific supplement, verifying that the product contains a clinically studied strain is the standard worth following. Monthly costs for probiotic and postbiotic products typically range from $15 to $40. For individuals with compromised immunity, postbiotics offer a safety advantage over live strains.
Frequently Asked Questions
Can postbiotics replace conventional acne treatment? Not at this point. Postbiotics are being studied as a supportive approach that modulates inflammation through the gut-skin axis, not as a replacement for retinoids, antibiotics, or other established therapies. If you are undergoing treatment, discuss adding any supplement with your dermatologist.
Which strains have shown effects on acne-related skin outcomes? L.plantarum HY7714 has data showing improved skin elasticity and reduced wrinkle depth. L.paracasei CNCM I-5220 demonstrated anti-inflammatory and barrier-protective effects. However, large-scale acne-specific trials are still lacking.
Should I choose probiotics or postbiotics? For those with compromised immunity or a weakened gut barrier, postbiotics may offer a safety advantage since they contain no live organisms. Healthy adults can consider either option, selecting based on strain name and available clinical evidence.